Exertional Shin Pain: Causes, Symptoms & Treatment

Pure Sports Medicine
- 21 September, 2018
- Podiatry
- Pain Management
- 2 min read
Medial Tibial Periostitis/Stress Syndrome (MTSS): MTSS is a condition involving the muscle origin, along the inner/front part of the shin. This is thought to arise from increased pulling or traction at the interface of the muscle on the bone, causing common symptoms of localised inflammation of the periosteum (lining of the bone).
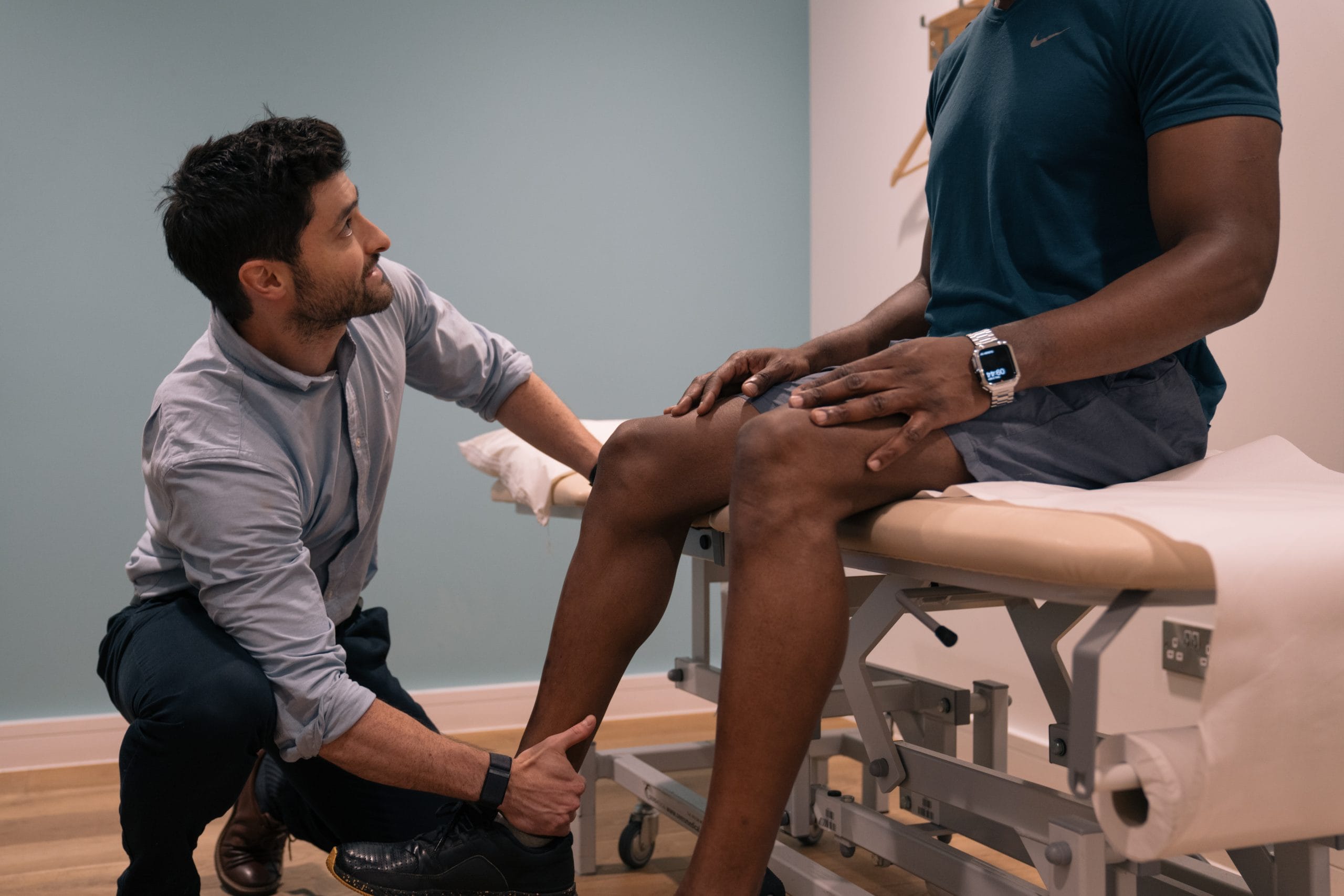
It is the most common cause of exertional shin pain and is frequently associated with tender leg pain, boggy swelling along the inside of the shin (bottom 1/3rd towards the ankle). This type of shin pain tends to ‘warm up’ with exercise, but excessive activity may lead to a deterioration of symptoms. MTSS tends to settle with relative rest, but it is essential to address any underlying predisposing factors, such as abnormalities of running mechanics, prior to return to training.
Stress Fracture
Bone is a tissue that is in a constant process of being built up and broken down. These processes must be balanced to maintain optimum bone health. If there is insufficient building of bone due to inadequate calorie intake, metabolic abnormality, or increased breakdown due to a change in training intensity, frequency or volume, the net result will be a reduction in bone density and a propensity to a bone stress injury, i.e. bone stress reaction or stress fracture. This type of shin pain tends to worsen with activity to a point where physical activity must be stopped to alleviate discomfort. It may affect the inner or front part of the shin and may be associated with localised bogginess or swelling. Pain that causes the individual to wake from sleep at night would raise a suspicion of a bone stress injury. Management initially involves reduction of load and stress upon the bone, usually in the form of an air cast boot, with or without crutches. Bone stress (reaction/fracture) is a serious injury and should be diagnosed early to avoid progression and long-term consequences.
Chronic Exertional Compartment Syndrome (CECS)
CECS is thought to occur because of tightness and reduced compliance of the fascia surrounding the muscles, most commonly the extensor muscles (that lift the foot up) in the front of the shin. Pain tends to build up as a pressure-type discomfort with ongoing impact activity, most commonly in the compartment on the outer part of the shin. This eventually reaches a point where the individual is unable to continue running and is forced to stop and rest. After several minutes, they are able to set off again. Individuals often have little pain at rest, other than tightness and mild discomfort in the affected compartment. Diagnosis relies heavily on a full exploration of the history and symptoms and may require the clinician to observe the individual during and after a run.
Exertional shin pain is likely to respond well to a multidisciplinary approach: involving doctors, physiotherapists, podiatrists, nutritionists, soft tissue therapists and strength and conditioning input.
If you have exertional shin pain, please feel free to book an appointment with Dr Thing or another of our clinicians.

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs