What is Plantar Fasciitis?

Claire Small
Chief Clinical Officer & Consultant Physiotherapist
- 28 March, 2025
- Podiatry
- 2 min read
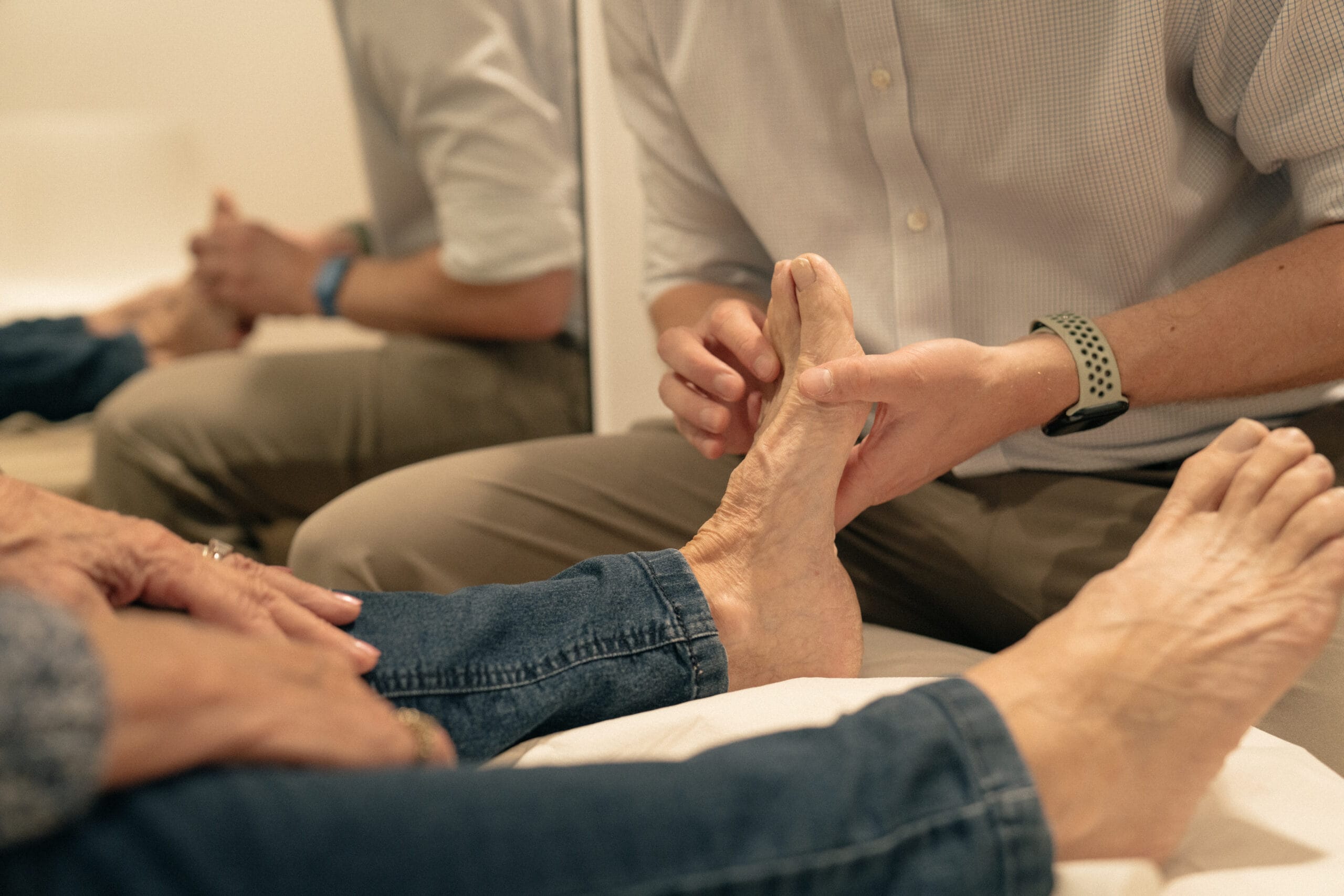
Plantar ‘fasciitis’ is a term commonly used to describe pain in the sole of the foot and inner border of the heel. This condition is thought to be due to ’overload’ associated with increased training volume in the athletic population, especially runners and dancers, but also due to lifestyle factors.

The condition is typically characterised by pain just below the heel or along the arch of the foot after a prolonged period of rest i.e stepping first thing in the morning which then eases with movement but exacerbated by prolonged periods of acitivities like walking, standing or running.
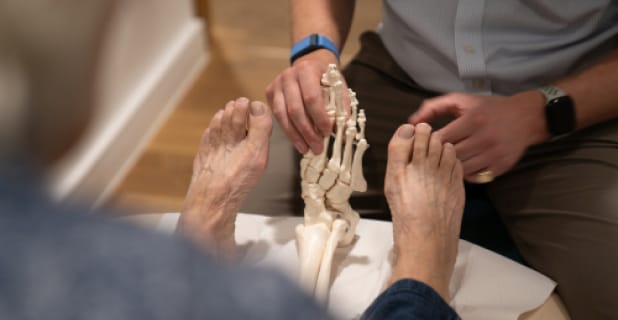
The plantar fascia is a thick band of fibrous tissue that is attached to the heel and to the base of the toes. Its function is to help support the medial arch along with intrinsic foot muscles via the Windlass mechanism. This mechanism is the tightening of the fascia when our toes bend backwards creating increased tension within it.
Although the term fasciitis implies inflammation, recent literature has suggested that the pathology resembles that of a tendinopathy with thickening of the fascial attachment, changes in the collagen structure and sometimes underlying bone oedema so it should be really be addressed to as fasciosis or more simply ‘plantar heel pain’. There are several other structures around the heel that can also be affected e.g. the fat pad, bursa, tendons, nerves. The exact diagnosis will depend on history, clinical examination and may sometimes involve imaging.
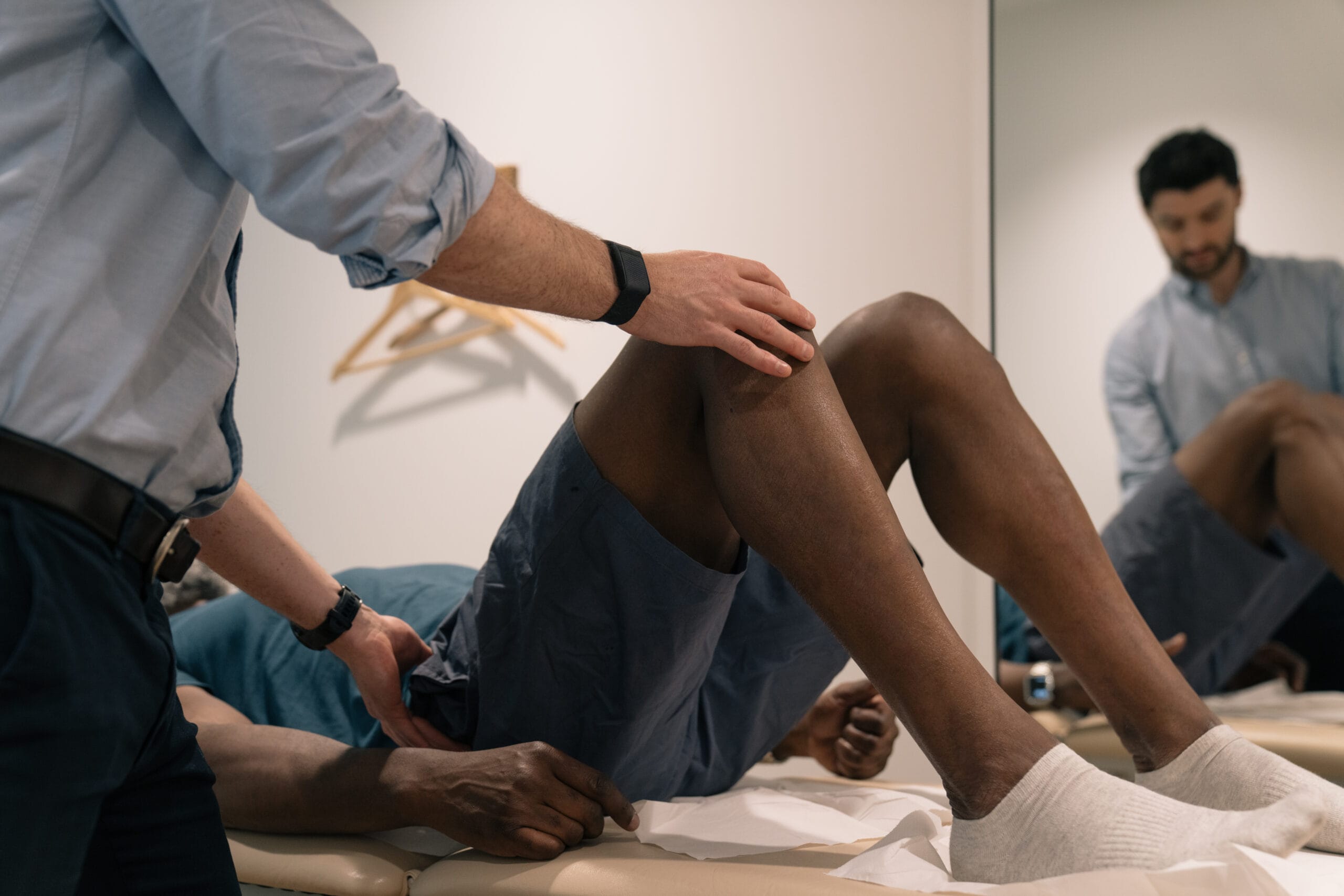
Factors associated with this condition are reduced ankle range of movement, tight calf muscles and weakness of the intrinsic foot muscles.
Treatment options commonly used are the use of gel heel cups which can be bought over the counter, regular stretching of the fascia and calf muscles. Sports Doctors can also be facilitated for onward investigations, and based on the assessment Podiatrists can also provide added valuable input for the tight musculature and custom insoles.
Interesting recent studies have shown changes in pain and function following high load strength training similar to treatment of tendinopathies. Strengthening of the hip muscles which control the movement in the knee and foot, helps to decrease the load on the fascia and has shown beneficial effects.
If you are experiencing pain in the sole of your foot and concerned it may be plantar fasciitis, and would like to speak to a specialist, click the button below.
References
- Riel H, Cotchett M, Delahunt E, Rathleff MS, Vicenzino B, Weir A, et al. Is ‘plantar heel pain’ a more appropriate term than ‘plantar fasciitis’? Time to move on. Br J Sports Med. 2017.
- Rathleff MS, Molgaard CM, Fredberg U, Kaalund S, Andersen KB, Jensen TT, et al. High-load strength training improves outcome in patients with plantar fasciitis: A randomized controlled trial with 12-month follow-up. Scand J Med Sci Sports. 2015;25(3):e292-300.
- Huffer D, Hing W, Newton R, Clair M. Strength training for plantar fasciitis and the intrinsic foot musculature: A systematic review. Phys Ther Sport. 2017;24:44-52.
- Kamonseki DH, Goncalves GA, Yi LC, Junior IL. Effect of stretching with and without muscle strengthening exercises for the foot and hip in patients with plantar fasciitis: A randomized controlled single-blind clinical trial. Man Ther. 2016;23:76-82.
- Plantar Fasciitis: Will Physical Therapy Help My Foot Pain? J Orthop Sports Phys Ther. 2017;47(2):56

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs