Restless Legs Syndrome

Pure Sports Medicine
- 27 February, 2019
- Lower Limb
- Podiatry
- 3 min read
Restless Legs Syndrome
Restless legs syndrome (RLS) is a common, sensorimotor, circadian sleep disorder characterized by the urge to move the legs. Abnormal sensations that start at rest but are improved by activity, symptoms are often worse at night with improvement in the morning (Romenets and Postuma 2013).
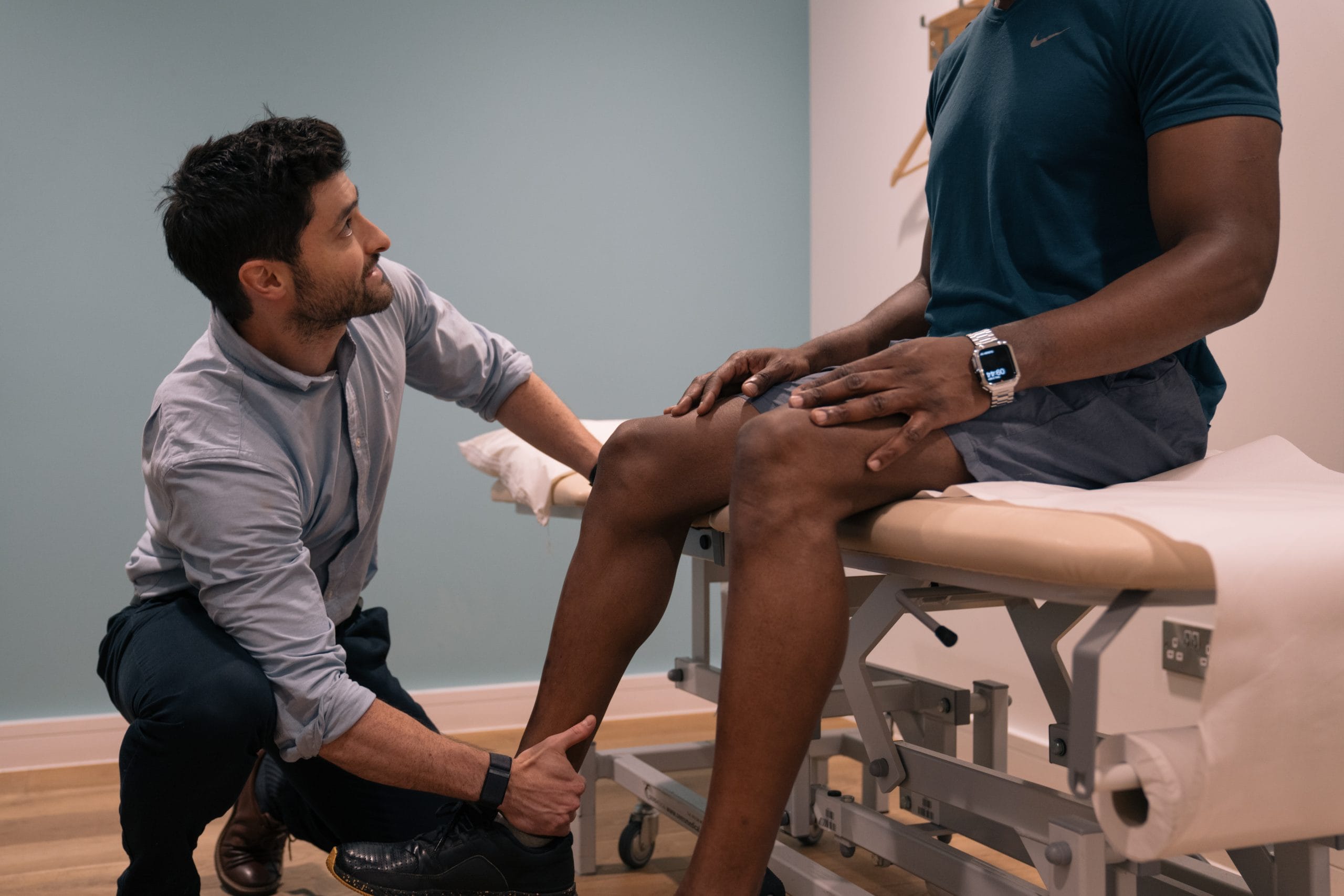
Soft Tissue Therapy and the treatment/management of RLS
When treating RLS, it is always advisable to first seek the patients’ doctor’s approval. The medical community regards restless legs syndrome as a condition that can be managed but not necessarily cured. In general, the therapeutic approach is dependent on improvement of the primary condition and the severity of the RLS.
In their study, Russell (2007) found that soft tissue therapy progressively increased the subject’s quality of life by allowing her to feel more rested and get more work done; she also reported that the effects of massage reduced symptoms of RLS. The results of this study revealed two improvements: a reduction in restless leg symptoms and the unforeseen result of warmer feet.
If medications are not used, most healthcare providers advise one or more of the following approaches:
- Massage – regular leg massage has been reported to ease RLS
- Hydrotherapy – Advising clients to take a warm bath often demonstrates favourable results. On the other hand, some people find relief with the application of cold packs
- Moderate Exercise – While moderate exercise early in the day benefits leg circulation and, therefore leg pain, strenuous exercise could potentially aggravate RLS
- Avoid Alcohol, Caffeine and Nicotine – Refraining from these substances, especially in the evening, can help reduce RLS severity
- Compression – Wrapping the legs in ace bandages or wearing compression socks or stockings can reduce RLS sensations
Soft tissue therapy is one of the most well-known approaches for helping RLS. Concentrating on the lower half of the body with special attention to releasing the piriformis muscle typically yields dramatic improvement in symptoms. Increasing circulation in the hamstrings can also relieve uncomfortable sensations in the legs. However, beware that deep relaxation may aggravate the condition.
Some favoured modalities for preventing the energetic accumulation common with RLS are myofascial release, trigger point therapy, deep tissue massage and sports massage techniques. Although there is no surefire way to get rid of RLS, soft tissue therapy is one of the most effective ways to deliver relief and reinstate a healthy sleep schedule.
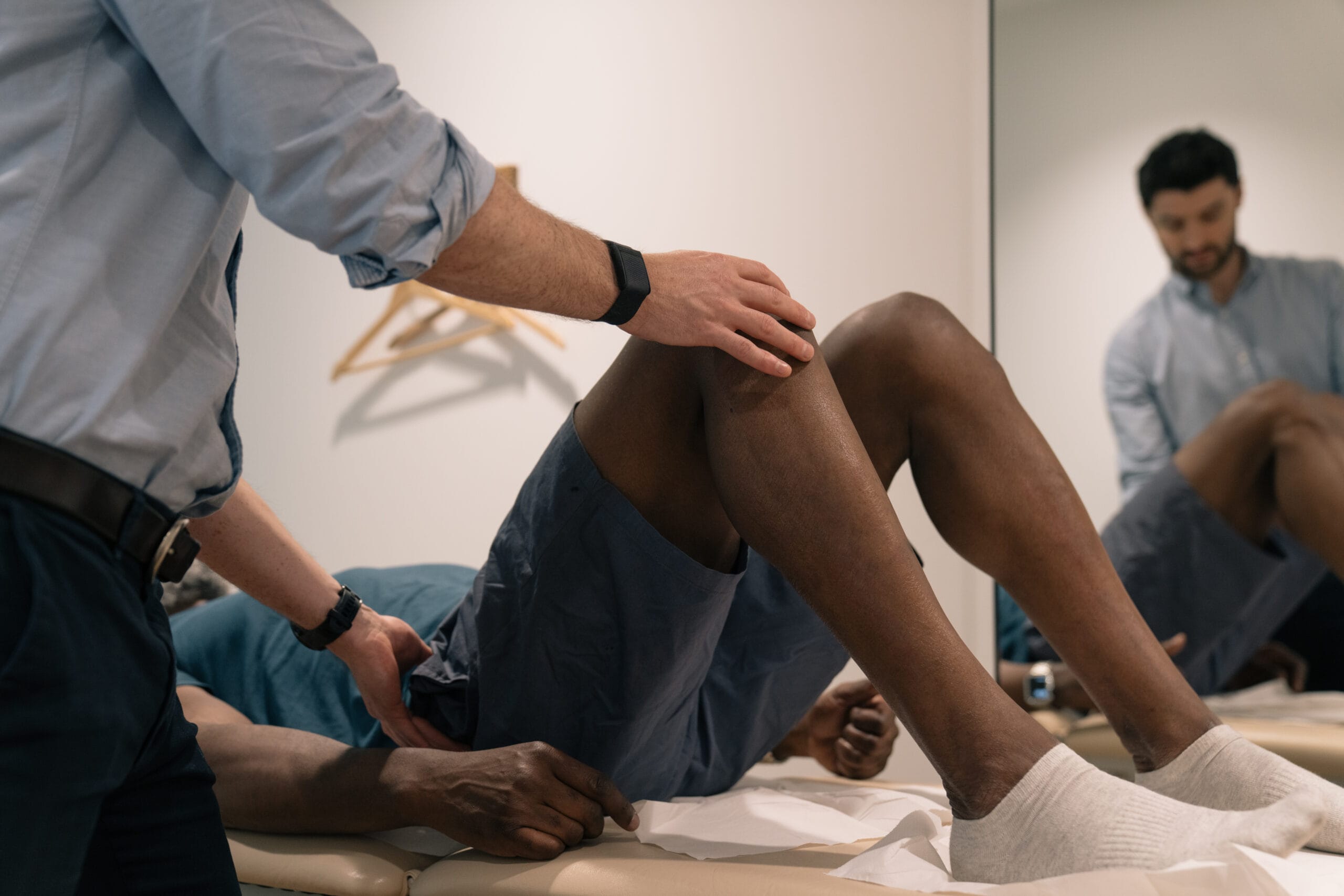
Although the symptoms can be different for each person affected, most people with RLS experience the following:
- Irritation – Leg sensations are often irritating, typically described along the scale from painful to uncomfortable. Although sensations are often in the calf area, some people experience them in the feet, upper leg, arms or even the hands.
- Need to move – People with RLS often have an overwhelming urge to move. Typically, getting up and moving around can relieve the discomfort.
- Position and time variables – The discomfort of RLS tends to increase when a person is in a sitting or lying down position. The intensity usually escalates in the evening or at night.
- Visible Movement – When a person with RLS sits or lies down, the movement or jerking of their feet or toes may be witnessed by others.
It is important to differentiate primary and secondary RLS from other conditions, which can mimic the symptoms of RLS, in particular neuropathy and cramps. However, despite considerable advances, the understanding of RLS pathophysiology remains incomplete. According to Romenets and Postuma (2013) there is insufficient evidence at the moment to recommend changes in lifestyle, nutritional supplements and any specific no pharmacologic treatments.
Although family history and high caffeine ingestion may cause RLS, the aetiology is unknown in most cases. Restless legs syndrome can also be a secondary problem brought on by other conditions. Examples include:
- Chronic Disease – An underlying medical problem, such as diabetes mellitus, kidney disease, Parkinson’s disease or rheumatoid arthritis could precipitate RLS.
- Pregnancy – Many women experience RLS in the last months of pregnancy. This may be related to an iron deficiency. Left untreated, the symptoms often go away after delivery.
- Iron Deficiency Anaemia – A lack of iron in the blood may not allow a muscle to rest.
- Neurologic Lesions – People with spinal cord tumors, peripheral nerve lesions or spinal cord injury often report symptoms of RLS
- Drug Side Effects – Medications including tricyclic antidepressants, anti-nausea and anti-seizure drugs, selective serotonin reuptake inhibitors (SSRIs), lithium, and some cold and allergy drugs may increase or trigger RLS symptoms. In addition, withdrawal from sedatives may trigger RLS
- Other conditions suspected of contributing to RLS include sleep apnea, narcolepsy, varicose veins, thyroid problems or problems with hand or feet nerves.
If you want to book an appointment with Shaun or another member of our soft tissue therapy team, follow the link or call your preferred clinic.
References
Cutler, N. (2007) 5 Bodywork Tips for Restless Legs Syndrome, Institute for Integrative Healthcare Studies, online 2017; http://www.integrativehealthca…
Romenets, S. Postuma, R. (2013) Treatment of Restless Legs Syndrome, Current Treatment Options in Neurology, 15 (4), pp. 396–409
Russell, M. (2007) Massage therapy and restless legs syndrome, Journal of Bodywork and Movement Therapies, 11, pp. 146–15

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs