The Effects of Concussion on the Sensorimotor System: Overlapping Pathologies

Claire Small
Chief Clinical Officer & Consultant Physiotherapist
- 26 March, 2018
- Physiotherapy
- Concussion Clinic
- 6 min read
The Effects of Concussion on the Sensorimotor System: Overlapping Pathologies
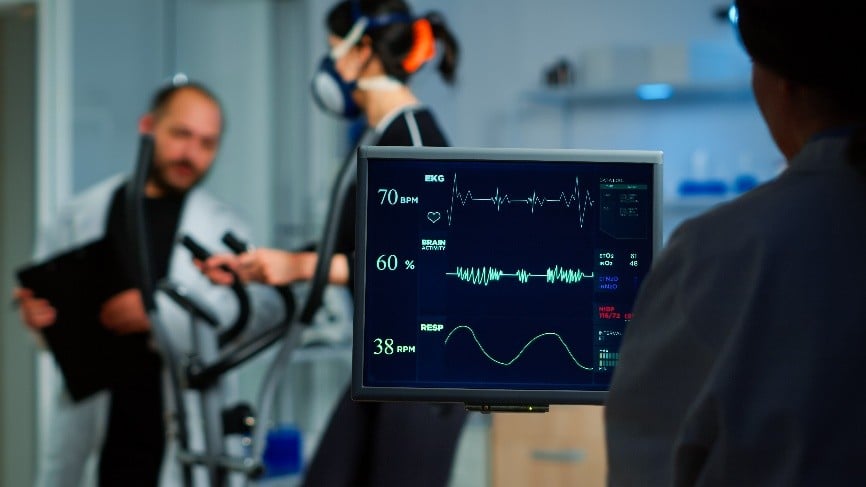
Welcome again to this week’s publication of The Concussion Blog. From the topics we’ve looked at so far in this series of blogs, it’s clear that concussion is a multi-faceted condition involving layers of overlapping pathologies that combine under normal circumstances to provide postural stability, balance, gaze fixation and positional sense.
So what happens to the vestibular and oculomotor systems, sway velocity, cervical proprioception and the trunk stability muscles in elite athletes following concussion? How do these systems interact? and how do they recover relative to one another?
This week, we’re going to consider a review by Hides and colleagues from Brisbane who conducted a prospective study looking at how sports concussion changes the sensorimotor system and the ways in which it recovers.
Hides J, Franettovich Smith M, Mendis M, Smith N, Cooper A, Treleaven J, Leung F, Gardner A, McCrory P, Low Choy N. A prospective investigation of changes in the sensorimotor system following sports concussion. An exploratory study. Musculoskelet Sci Pract. 2017 Feb 24;29:7-19.
Symptoms of dizziness and balance dysfunction are some of the most common concussion symptoms and strongest predictors of prolonged recovery following concussion(2). These symptoms are linked (although not exclusively) to deficits in the somatosensory system. With that in mind, looking at tests such as trunk and cervical proprioception, trunk muscle tone and the vestibular system (although not directly part of the somatosensory system, it has a strong link to it through cervical afferents) can directly influence our management choices.
The somatosensory system is a system that relays sensations detected in the periphery and conveys them via pathways through the spinal cord, brainstem, and thalamic relay nuclei to the sensory cortex in the parietal lobe.
During a concussive event, damage can occur to the vestibulo-ocular system as well as the afferent input from the cervical spine. The altered messages arising from these systems can lead to changes in the efferent input to the somatosensory system, and a crescendo of maladaptive patterns may occur. This may lead to further deficits in balance, proprioception and body position that, if unaddressed, may leave athletes vulnerable to further concussive and non concussive injuries.
Force of impact has been shown to be reduced by 67% when the head is aligned with the torso(5), and the contractile ability of the lumbar multifidus muscles has been found to be a predictor in head and neck injury in AFL players(3). Adequate proprioception of cervical and lumbar trunk muscles helps to minimise injury by enhancing the player’s ability to pre-set the head in an optimal position(4). These muscle groups are largely modulated by the vestibulo-spinal system, where alteration in input can lead to changes in the deep cervical and trunk muscles.
Methods
Hides and her team conducted a prospective cohort study of 54 professional rugby union and league players. Each player was assessed for cervical proprioception, balance, vestibular function and trunk muscle size pre season and then again following concussion. The concussion diagnosis was made by the club medical staff and the independent match doctor. There were no control athletes in this study as all athletes were deemed to act as their own ‘control’ using pre season and post injury measures.
Balance
Each athlete completed the Stability Evaluation Test (SET), conducted under six stance conditions- (20s each) without foot-wear: feet together, single leg stance (standing on non- dominant leg) and tandem stance (non-dominant foot behind) on firm, then foam, surfaces using the VSR sport balance evaluation system. From this system, sway velocity was taken. Sway velocity measures the average horizontal area covered by movement of the centre of force per second.
Vestibular
Vestibular and oculomotor assessment was conducted using a test battery of Head thrust test for visual-ocular reflex, smooth pursuits, saccades and gaze stabilization for vestibular-oculomotor dysfunction and the Dix-Hallpike and head roll tests for BPPV (BPPV is present in only 5% of concussions). Frenzel goggles were used to look for nystagmus, but this can be done effectively with the naked eye, which is significantly cheaper!
Cervical spine proprioception testing
Cervical spine joint position error scoring was used to assess cervical stability. This is a really useful and simple tool to asses cervical proprioceepion, all you need is a lazer pointer that fixes to the head and a white board with some targets drawn on it. The scoring protocol can be found online and involves rotating the neck with the eyes closed and attempting to return to cervical neutral without using vision.
In this test, the researchers reversed the protocol by attaching a laser pointer to the sternum and moving the trunk on a static head as opposed to the head and neck on a static trunk. This was to avoid head movement and thus take the vestibular system out of the equation. Personally, I think this test will assess thoracic proprioception rather than cervical and haven’t been able to find any literature that validates this protocol.
Trunk muscle cross sectional area
The multifidus muscles were imaged from the L2 to L5 vertebral levels, and the quadratus lumborum muscle was measured at L3-4 vertebral interspace. Further thickness measures were taken at the transvers abdominis, internal obliques and multifidus at rest and on contraction.
Results
Of the 54 players with a mean career length of 6 years, 14 concussions were recorded. Three players suffered repeat concussions, and their second concussion wasn’t analysed. This left 11 players that had repeated posts concussion assessments. No players presented with symptoms of BPPV.
Balance
The mean of the six test conditions tested during the Balance Evaluation Test for postural stability revealed reduced sway velocity post concussion (p=0.02), but none of the individual components were significant on their own.
Vestibular
Five athletes developed post concussive vestibular signs that were deemed to be out of the normal clinical range. Although this was not found to be significant when looked at as a whole group, this is probably an accurate representation of the prevalence of vestibular and oculo-motor pathology experienced post concussion (Visual Motion Sensitivity present in 49%, Alsalaheen 2010). There is a significant body of evidence that supports the presence of vestibular and oculo-motor dysfunction post concussion, including two studies we have reviewed in this blog series (see blogs 1 and 5). As we know,w vestibular and oculomotor dysfunction can lead to symptoms of dizziness and impaired balance. Not assessing these systems, even if the athlete has achieved full symptom recovery, leaves athletes open to significant injury following a return to play.
Cervical proprioception
No significant difference was seen in cervical proprioception pre and post concussion. Looking at the methodology of this study, I think it has more to do with the fact that the researchers assessed thoracic proprioception more than they did cervical, so we’ll move on from this and not let it ruin the rest of the paper!
Trunk muscle cross sectional area
Significant increases in multifidus CSA were noted at right L4 and bilateral L5 (p=0.02 and 0.05 respectively). The right external oblique was also found to be increased in CSA (p=0.01).
Discussion
When I read this article initially, I was skeptical on two main points- firstly, lower limb and back injury incurred during the season was going to affect sway velocity and abdominal muscle thickness, and secondly, won’t being mid season naturally lead to abdominal muscle thickness through increased activity and hypertrophy? In fact, it was reported that no concussed players reported lower back or lower limb injury that could confuse the findings of the study, and most interestingly, longitudinal studies have demonstrated that multifidus muscle CSA actually decreases across the playing season(3)
This study demonstrates the presence of neuromuscular changes following concussion with significant decreases in sway velocity and an increase in abdominal muscle cross sectional area (which we are extrapolating to an increase in tone). The exact mechanism for this is unknown. I think it’s likely that this was either related to a compensatory mechanism of splinting of the trunk or an alteration of the efferent input to the trunk stabilisers following abnormal afferent input from the cervical spine and vestibulo-oculomotor system.
Athletes post concussion may adopt a strategy of splinting to compensate for reduced balance and in doing so reduce their postural sway. This is also consistent with increased CSA of trunk stability muscles post concussion. These two factors on their own aren’t remarkable, but when you consider them to be part of a larger system that demonstrates less capacity to compensate for postural adjustments and potentially absorb force when tackled, they become worth thinking about.
Stay in touch:
Twitter: @Theo_Farley
Email: [email protected]
To book an appointment with Theo, either follow the link or call our Kensington clinic.
References
- Alsalaheen, BA., Mucha, A., Morris, LO., Whitney, SL., Furman, JM., Camiolo-Reddy, CE., Collins, MW., Lovell, MR., & Sparto, PJ. (2010). Vestibular rehabilitation for dizziness and balance disorder after concussion. Journal of Neurologic Physical Therapy,34, 87-93.
- Ellis, M. J., Leddy, J. J. & Willer, B. 2015. Physiological, vestibulo-ocular and cervi- cogenic post-concussion disorders: an evidence-based classification system with directions for treatment. Brain Inj., 29 (2), 238-248.
- Hides, J. & Stanton, W. 2012. Muscle imbalance among elite Australian rules football players: a longitudinal study of changes in trunk muscle size. J. Athl. Train, 47, 314e319.
- Pinsault, N., Anxionnaz, M. & Vuillerme, N. 2010. Cervical joint position sense in rugby players versus non-rugby players. Phys. Ther. Sport, 11, 66e70.
- Viano DC, Pellman EJ. Concussion in professional football: biomechanics of the striking player: part 8. Neurosurgery. 2005;56:266–280.

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs