What are Stress Fractures?

Dr James Noake
Consultant in Sport, Exercise & Musculoskeletal Medicine
- 26 June, 2018
- Sport, Exercise & Musculoskeletal Medicine
- Strength & Conditioning
- 4 min read
What are Stress Fractures?
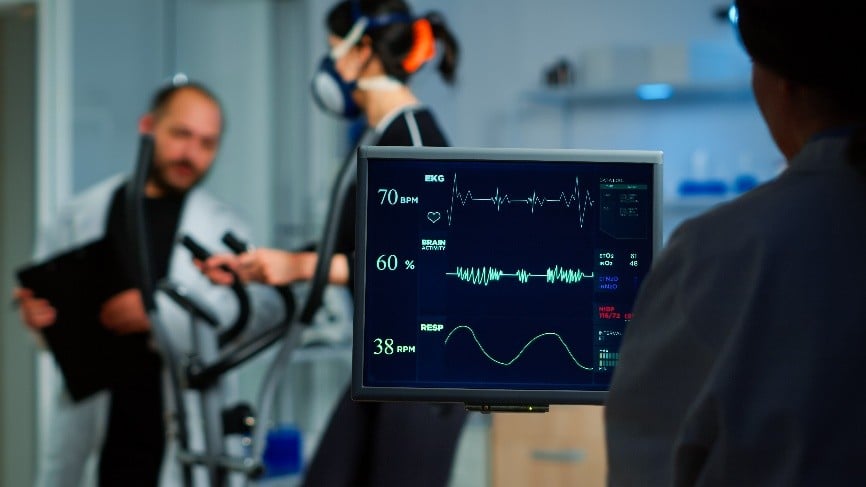
A stress fracture is a break that can occur in a bone due to load or insufficient energy absorption rather than direct trauma like other fractures. A stress fracture is part of a spectrum – at one end, it would be graded as a stress response and at the other, a stress fracture with a true fracture line. Patients can present at any point on the continuum, and the good news is that the earlier it is detected, the quicker the recovery.
We often think of bones as inert, but they will react to load just like muscles, tendons and ligaments. As part of the homeostatic process to maintain healthy bones, there is a cycle of bone being broken down by cells called osteoclasts and built up by osteoblasts. When there is a greater rate of bone being broken down compared to that being built up, an imbalance is created, which can lead to a stress fracture.
The diagnosis of a stress fracture will mean several months out of impact training and then several months to return. So, understanding how they occur can be a useful way to prevent them.
Symptoms / Diagnosis

Pain from a stress fracture can present in different ways. Most often, it starts as a low level dull ache in the affected area, becoming increasingly severe if the patient ignores the symptoms and continues to exercise and load the injured body part, preventing it from healing.
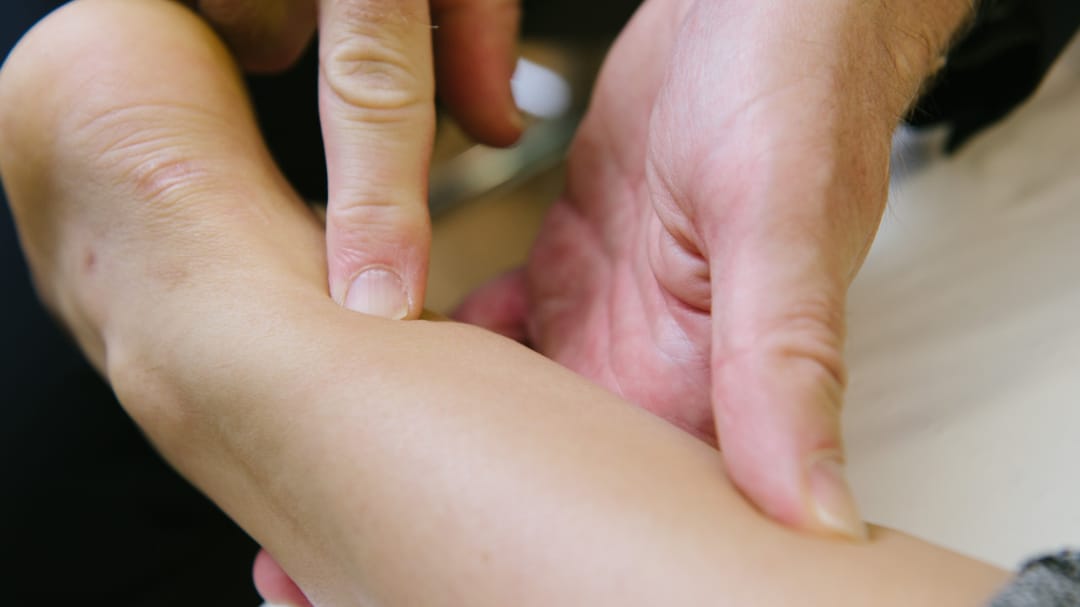
If there is inflammation of the lining of the bone (‘periosteum’), then it can be very painful to touch and feel swollen compared to the other side. However, the pain can also sometimes radiate (‘refer’) outwards from the stressed bone, perceived diffusely in a wider area, which sometimes makes it hard to localise and can make the diagnosis unclear in some cases.
It can persist after provocative activity, and pain at night or rest is a typical feature. It can last for several days after an intense period of exercise, and as the stress injury becomes more established, it can be intrusive even on simple daily activities such as walking to and from work.
A stress fracture can be missed on a simple x-ray, especially if the injury is less than 2 weeks old. After this period, changes can be seen on the x-ray images with swelling of the lining of the bone and ‘haziness’ around the site, indicative of the bone attempting to heal.
MRI scanning is a much more accurate method to pick up a stress fracture; even subtle bone stress can be identified, allowing early diagnosis and, therefore, improving prognosis and recovery times. MRI also shows associated soft tissue problems and inflammation that can co-exist with the bone stress and which can complicate the treatment plan.
CT scanning gives excellent bony detail and anatomy and is used in the assessment of high risk stress fractures, if the stress fracture is particularly complex or advanced, or if there is any suggestion that the stress fracture is failing to heal (‘delayed or non union’)
Causes

The causes can be multifactorial. The extrinsic factors would include training volume and intensity, recovery between sessions, sleep, footwear, training surface, etc and intrinsic factors would relate to the body and how a person moves, ie biomechanics. It may be that there are areas of weakness, inflexibility or poorer patterns of movement that contributed to overload.
Stress fractures, particularly in females, appear to be secondary to dietary and endocrinological problems that commonly occur in females. Adopting restrictive eating behaviours will result in low energy availability. Low energy availability means you do not have enough calories (energy) for your body’s needs AND for exercise. Low energy availability ( < 30kcal/kg lean body weight (LBW)) has been shown to disrupt reproductive and metabolic hormones, which in turn decreases the body’s ability to build bone, maintain muscle mass, repair damaged tissue and recover from injury. Research has shown that bone formation is impaired within 5 days of the onset of low energy availability.
Specific nutrients also play a role in stress fracture risk in both male and female runners. A diet with inadequate protein, calcium, potassium, vitamin D and K, regular intake of carbonated drinks, caffeine, and alcohol are all linked to lower bone mineral density. Moreover, poor nutritional habits also hinder the ability of bone to repair and maintain itself as the components needed in the healing process are not present in sufficient quantity.
Treatment & Management
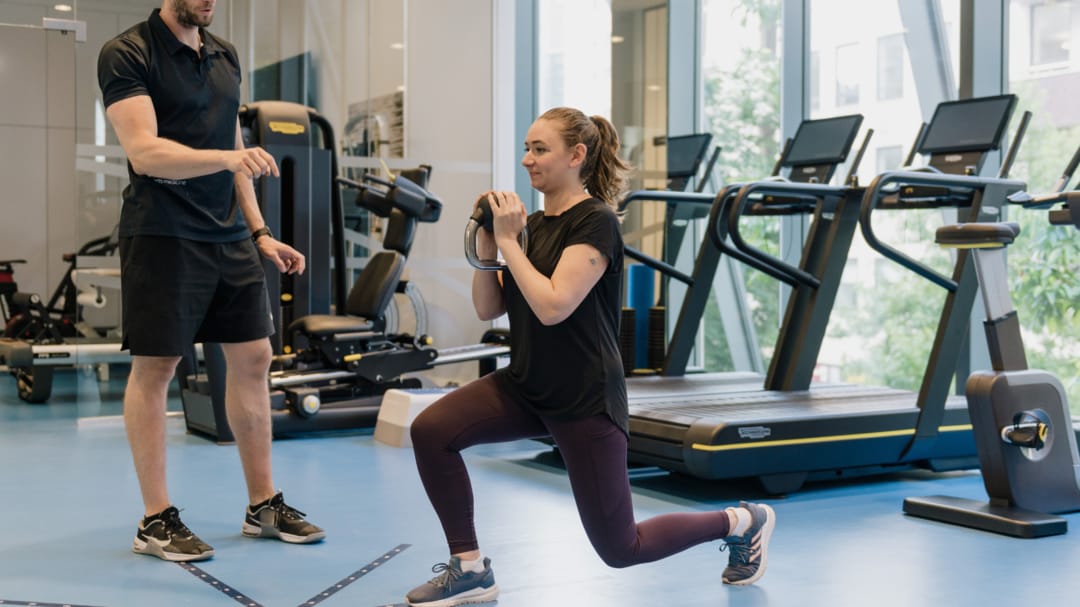
A multi-disciplinary team approach is recommended for the management of stress fractures. A patient would typically get input from a Sports Doctor, Dietitian and Physiotherapist and may also need Podiatric input as well if their foot posture is a concern.
Initially, the bone needs to have a phase of reduced load, and this would be avoidance of any impact and may even involve a period of time using crutches or an orthopaedic boot until walking and activities of daily living are pain-free. During this time, the causes of the stress fracture will be examined. For a lot of patients, this means looking at several different factors, from their biomechanics and training load to nutrition or supplementation. To support the healing process, it is important to maintain adequate energy availability. It is also vital to balance the intake of carbs, protein and fat as well as ensure micronutrient requirements (such as vitamin D, vitamin K, calcium, phosphorus and magnesium).
From the outset, a patient would work with the Physiotherapist to correct any biomechanical contributing factors as well as discuss and learn the role of the extrinsic factors. More load would be gradually introduced as the stress fracture was healing initially through the re-introduction of day-to-day activities and ultimately resistance exercises. This often takes several weeks.
Finally, a structured return to the running program would be developed. The amount of time a person has to be out of running will depend upon their biomechanics, degree of the stress fracture and the speed they are able to return to pain-free day to day activities.
If you’re concerned that you may have a stress fracture and would like to speak to a specialist, get in touch today.

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs