Kate’s Story

Dr Sarah Rollins
Consultant in Sport, Exercise & Musculoskeletal Medicine
- 10 August, 2024
- Pregnancy
- Consultant Specialists
- SEM
- Women's Health
- 1 min read
After struggling to regain strength and range of motion of her abdomen and pelvic floor following pregnancy, Kate was concerned that she was out of options. But she didn’t give up and sought the help of our Women’s Health team who offered the care and support Kate needed.
Following the birth of my second daughter almost 6 years ago I struggled with my core strength.
For me this presented in several ways – lower back pain, rib flaring and pain, shortness of breath, hip tension, tension at the back of my pelvis and urinary incontinence with some high impact activities such as running.
These symptoms limited the physical activities I could perform, but also significantly affected my mental health. It’s hard to put into words for anyone who has not experienced it, but it felt as if my body was at war with itself.
I was aware that I had separation of my abdominal muscles (‘diastasis recti’) as a result of my two pregnancies and, over the years, I saw a number of physiotherapists at different practices and postnatal personal trainers. I religiously practised the exercises they prescribed me and saw some short-term improvements but never felt any significant improvement in my symptoms. At times it felt as if the exercises actually made my symptoms worse.
From my experience, the information available to women around diastasis recti is somewhat lacking, or even at times unhelpful — even from professionals who are in theory trained to provide postnatal services.
I felt for a long time that something wasn’t right in my body and that things shouldn’t feel as hard as they did, but over the years I was repeatedly told that the size of the diastasis (the separation of my stomach muscles) was irrelevant and that the only thing that mattered was whether I could generate tension between the two sides of my rectus abdominis muscles. I was told that the tension down my midline was good and so I didn’t push harder for further investigation.

After 5 years of ongoing symptoms, I was left feeling lost. I was even told by some professionals that I just needed to “stop thinking about it” and that I was “too body aware” which left me feeling like it was all in my head or that I was asking for too much or looking for something that didn’t exist.
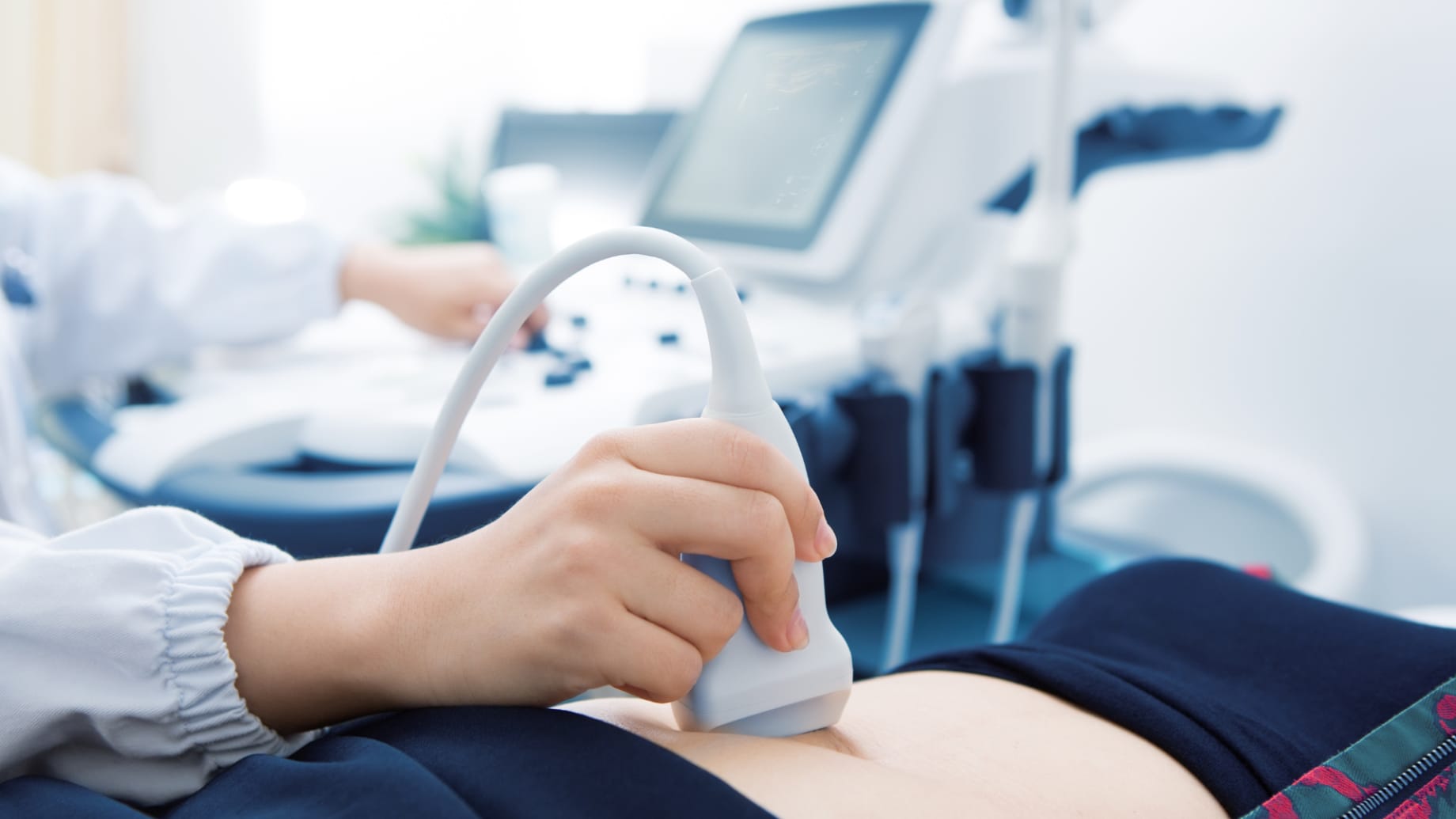
I sought help from Pure Sports Medicine about a year ago, initially from Physiotherapist, Alice Mason. After a few sessions I felt some improvements, but still felt frustrated that my symptoms were persisting. In February this year I went back to Alice and explained how despondent and frustrated I was feeling. She took the time to listen to me and referred me to Sport & Exercise Medicine Consultant, Dr Sarah Rollins, for an ultrasound of my anterior abdominal wall to try and get a clearer picture of what was going on.
At the appointment with Dr Rollins, she initially asked me about my symptoms and then performed an ultrasound assessment of my abdominal wall in standing and lying positions and with relaxed and contracted abdominal muscles.
She explained what she was doing throughout the assessment and clearly explained what the ultrasound was showing. In my case, the ultrasound showed a 5.5cm separation of my rectus abdominis which is considered ‘severe’. Understanding that I had already done over 5 years of physio and rehab, Dr Rollins recommended that abdominoplasty surgery would be the best course of action for me.
She highlighted what the surgery would involve, the recovery process and the expected benefits. I felt daunted at the prospect of a major surgery, but incredibly relieved that there was an explanation for all the difficulties I had been experiencing over the years and reassured that I finally had a plan and a support team.
Following an initial consultation with the surgeon I had a follow-up appointment with Dr Rollins to discuss some queries I had about the surgery and expected outcomes. My husband also attended as he had been unable to attend the initial ultrasound. We both found this appointment very reassuring.
The surgery has a 6‑week recovery time, and I was feeling a lot of guilt around putting my own needs above those of my family, particularly as the surgery isn’t currently covered by the NHS or private health insurance (which itself is a topic that warrants its own article!). Dr Rollins gave me the gentle reassurance I needed that it was ok to prioritise my health and hopefully come out stronger at the end. Mentally I felt better than I had done in years, feeling supported and knowing that there was some hope for an improvement in my symptoms.
I chose to proceed with the surgery which took place in mid-May. The first 2 – 3 weeks were the hardest as my tummy felt very tight and sore and my mobility was limited. However, I had expected this from my discussions with Dr Rollins and the surgeon, so it felt manageable.
I had arranged for a nanny to look after my children during the first few weeks after surgery, so I was able to focus on my recovery. I had a check-ups with the surgeon after 10 days and 6 weeks, and a telephone check-in with Dr Rollins after 2 – 3 weeks, so I felt well supported.

I am now 10 weeks post-surgery and I have started a rehab physio programme with Alice. There is still work for me to do in correcting old and unhelpful movement patterns that my body developed over the past 5 years, but I can already feel the difference when performing the exercises I have been prescribed.
I can feel a much better connection between the top half and bottom half of my torso; my shoulders and neck feel less tense and my pelvic floor muscles feel more integrated with the rest of my core. I now have hope and belief that I will be able to progress over the coming weeks and embark on the higher intensity activities that were previously not possible for me.
Surgery will not be necessary or the right approach for everyone with a diastasis. However, I feel that it is an option that should be discussed more openly in relation to diastasis recti without the assumption that abdominoplasty surgery would only be for aesthetic reasons.
Even just a few weeks after the surgery I can feel the functional benefits. In my case, being able to quantify the size of my diastasis through an ultrasound assessment was invaluable and gave me the information and confidence I needed to do something different and embark on surgery.
It feels like the start of a new chapter in my life, and I feel very grateful to Dr Rollins and Alice at Pure Sports Medicine.
If you would like more information on our Women’s Health service, please click the button below.

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs