The Mind-Body Connection; Exercise, Pain and Mental Health

Pure Sports Medicine
- 30 September, 2019
- Exercise
- 3 min read
We all know the benefits that physical activity can have on our bodies, and that it decreases the likelihood of developing many chronic conditions like heart disease, obesity, osteoporosis and cancer; just to mention a few. However, not only does your body benefit from exercise, but there is now a significant body of evidence supporting the link between physical activity and mental health.
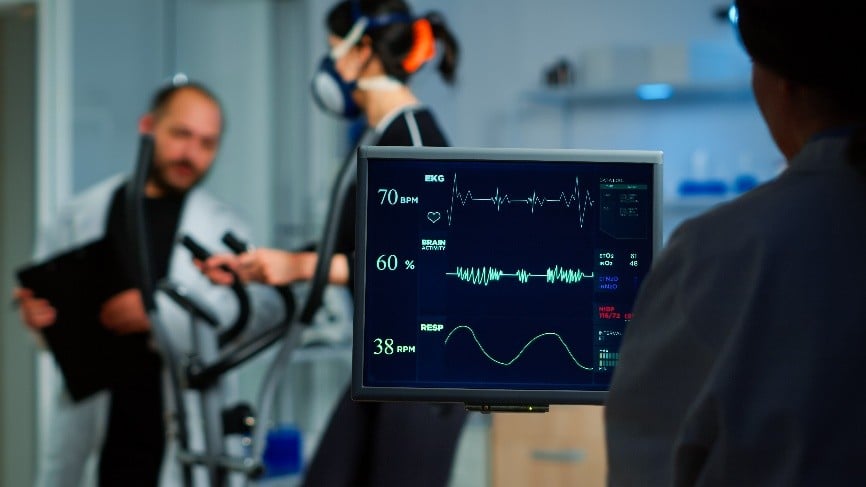
The research supports exercise prescription in the treatment of both chronic pain patients and those suffering from a variety of mental health conditions, such as anxiety, depression and even schizophrenia.
The mind-body link is integral to overall wellness and understanding this connection can help many people achieve a healthier, longer, and better quality of life.
When people come into our clinics across London, they are usually in some form of physical pain and dysfunction, usually resulting from injury or the normal aging process. They come to see our specialised team to have treatment and to have a clearer understanding of what is happening in their bodies.
For example, if you hurt your shoulder playing tennis, you might need imaging such as an MRI, and depending on the diagnosis a concise treatment plan will be created. In these instances you would need to see a Consultant in Sport & Exercise Medicine

However, some conditions are more complex or potentially chronic, and are affected by a variety of factors, including a how you are feeling.
This is not to say that physical symptoms are not real, or that they are ‘all in your head’, it simply means that our thoughts, feelings, attitudes and beliefs can positively, or negativity, impact the physical health of our bodies.
The way we care for our physical bodies (diet, exercise, sleep, alcohol intake etc) affects our state of mind and it is a complex interrelationship. Wellness is a dynamic active process which includes the ‘whole’ person.
The body communicates with itself constantly; the nervous system, the circulatory system, the immune system etc. all use a shared chemical language to maintain homeostasis. One component of this language are endorphins, they are self-made brain chemicals known as neurotransmitters.
They play a key role in how the body copes with pain and stress, for example with higher levels of endorphins less pain is felt, and the negative impacts of stress are decreased.
Increased endorphin production can come from many different external sources; chocolate, chilli, massages, sex and even hugs! One well documented source is exercise. Through physiological and biomechanical processes there is a cascade of positive effects that ripple through the body during and post physical activity.
These Processes Have a Psychological Impact such as;
- Elevating your mood.
- Relieving stress.
- Improving sleep.
- Improving memory.
Additionally, Exercise Builds and Supports a Healthy Brain As It Decreases The Risk of:
- Cardiovascular disease.
- Obesity.
- Diabetes.
- Hypertension (which can cause neurodegeneration).

Mental Health and Physical Health are Directly Linked
We’ve all experienced periods of anxiety and situational depression, while others battle with ongoing mental health issue throughout their lives.
Many of these conditions can have symptoms such as: feeling hopeless and helpless, poor sleep, decreased concentration, irritable bowel or constipation, changes in appetite and even unexplained aches and pains.
There are a variety of anti-anxiety medications, anti-depressants and antipsychotics, all of which can have unfavourable side effects. For example; changes in energy levels, motivation, sex drive and appetite.
These can be barriers to exercising. However, even small amounts of physical activity can improve mood, sleep and perceived hopelessness. Endorphins flood the brain during and post exercise; our bodies’ natural ‘feel good’ chemicals.
Research into chronic pain and physical activity is still in its infancy, however there is already strong evidence to support exercise and the inhibition of pain.
Pain is usually associated with injured tissues, but this is not always the case as chronic pain is a complex multifactorial experience and is not always an accurate representation of tissues status.
Pain science now recommends a biopsychosocial approach, this means chronic pain can and is modulated through somatic (body), psychological and social factors.
It is not uncommon for chronic pain and mental health disorders to be experienced together, as the share a similar neural pathway. The stress of living in a state of pain can increase anxiety and lead to fear-avoidance behaviours.
We know that sedentary lifestyles increase the likelihood of developing a chronic pain condition, therefore increasing activity levels can be preventive. Research is now suggesting exercise can help to regulate pain perception, so people in chronic pain can feel more in control of their bodies and lives.
Physical activity guidelines recommend 150mins per week. That may sound like a lot, but if broken into small chucks is very achievable.
There are obvious lifestyle changes to increase activity, like buying a gym membership, taking up Pilates or joining a team sport. However even small changes can make a difference too. Such as; walking from the train station instead of taking the bus, using the stairs instead of the lift, engaging in frisbee or rounders etc instead of sitting in the park.
Every little bit counts. A healthy body, a healthy mind.

Advice
Over the last 20+ years our experts have helped more than 100,000 patients, but we don’t stop there. We also like to share our knowledge and insight to help people lead healthier lives, and here you will find our extensive library of advice on a variety of topics to help you do the same.
OUR ADVICE HUBS See all Advice Hubs